Botox Application Points: A Comprehensive Guide (Based on Available Information ─ 04/21/2026)
Botulinum toxin type A, commercially known as Botox, originates from the Clostridium botulinum bacterium, with documented use tracing back to 19th-century German medical research.
Botox, a widely recognized brand name for botulinum toxin type A, is a neurotoxin produced by the bacterium Clostridium botulinum. Its journey in medical application began in the 19th century with the work of German physician Justinus Kerner, who first documented its paralytic effects. However, its therapeutic potential wasn’t fully realized until much later.
The core mechanism of Botox revolves around its ability to block nerve signals. When injected, it prevents the release of acetylcholine, a neurotransmitter responsible for muscle contraction. This temporary paralysis is the foundation of its cosmetic and medical applications. Specifically, Botox binds to receptors on nerve endings, inhibiting the fusion of vesicles containing acetylcholine with the cell membrane.

This interruption of nerve-muscle communication leads to muscle relaxation, smoothing wrinkles, reducing muscle spasms, or controlling overactive glands. The effects are not permanent, typically lasting three to six months, as the nerve endings eventually regenerate and restore acetylcholine release. Understanding this mechanism is crucial for appreciating the diverse applications of Botox.
Historical Context of Botox Use
The story of Botox’s application extends back to the early 19th century, with Justinus Kerner’s pioneering research in 1820. He identified the toxin produced by the bacterium Clostridium botulinum as the cause of botulism, a severe form of food poisoning characterized by paralysis. However, it wasn’t until the mid-20th century that its potential therapeutic benefits began to emerge.
Significant advancements occurred in the 1950s with the work of Vernon Brooks and Edwin Schantz, who successfully isolated and purified the botulinum toxin. This purification paved the way for controlled clinical studies. Initially, Botox found its primary medical use in ophthalmology during the 1970s, specifically for treating strabismus (crossed eyes) and blepharospasm (uncontrollable eyelid twitching).
The pivotal moment for cosmetic applications arrived in the late 1980s when ophthalmologists noticed that Botox injections smoothed wrinkles around the eyes. This observation led to its FDA approval for cosmetic use in 2002, revolutionizing the field of aesthetic medicine and solidifying Botox’s widespread popularity.
Types of Botox Available (Botulinum Toxin Type A)
While commonly referred to as “Botox,” it’s crucial to understand that Botox is actually a brand name for a specific formulation of botulinum toxin type A. Several other brands utilize the same neurotoxin, offering clinicians and patients a range of options; These include Dysport, Xeomin, and Jeuveau, each with subtle differences in formulation and unit potency.
Botox, manufactured by Allergan, was the first botulinum toxin product approved by the FDA. Dysport, from Ipsen, generally requires a higher unit dosage for comparable effects due to its spread. Xeomin, produced by Merz Aesthetics, is unique as it’s a “naked” toxin, meaning it’s formulated without complexing proteins, potentially reducing antibody formation.
Jeuveau, by Evolus, is a newer entrant marketed specifically for cosmetic use. The choice between these brands often depends on individual patient needs, physician preference, and desired treatment outcomes. Understanding these nuances is vital for optimal results.

Facial Aesthetics: Common Botox Application Areas
Facial aesthetics leverage Botox to diminish wrinkles, targeting areas like glabellar lines, forehead creases, and crow’s feet for a rejuvenated, smoother appearance.
Glabellar Lines (“Frown Lines”) ― Detailed Application
Glabellar lines, often called “frown lines,” are a primary target for Botox injections due to their significant impact on perceived age and emotional expression. Successful treatment requires a precise understanding of the underlying musculature – primarily the corrugator supercilii and procerus muscles.
Injection points typically include the central glabellar region, carefully avoiding diffusion into the orbicularis oculi to prevent eyelid ptosis. Dosage varies based on muscle mass and line severity, generally ranging from 10-25 units total, split between several injection sites. A common approach involves 5 units each into the central and lateral portions of the corrugator, and 5-10 units into the procerus.
Careful assessment of the patient’s facial anatomy and dynamic wrinkles is crucial. The injector must observe the patient’s natural expressions to accurately identify the contributing muscles and tailor the injection plan accordingly, ensuring a natural and aesthetically pleasing result. Post-injection, patients should avoid rubbing the treated area for several hours.
Forehead Lines ─ Horizontal & Vertical
Forehead lines, encompassing both horizontal and vertical expressions, are frequently addressed with Botox to achieve a smoother, more youthful appearance. Horizontal lines arise from the frontalis muscle, while vertical lines, often termed “glabellar” when prominent, involve the corrugator supercilii and procerus muscles – though these are primarily discussed under glabellar line treatment.
For horizontal lines, injections are typically administered along the superior border of the brow, avoiding the brow itself to prevent unwanted drooping. Dosage generally ranges from 10-20 units, distributed across 3-5 injection points. Vertical lines require more nuanced targeting, often combined with glabellar treatment.
Precise injection technique is vital to maintain natural brow movement and avoid a “frozen” look. Careful assessment of the patient’s muscle activity during animation guides the injector’s approach. Post-treatment, patients should refrain from strenuous activity for 24 hours to optimize Botox diffusion and effect.
Crow’s Feet ― Periorbital Botox Application
Periorbital Botox application, targeting “crow’s feet,” aims to soften dynamic wrinkles radiating from the outer corners of the eyes. These lines are caused by the orbicularis oculi muscle contraction during smiling or squinting. Successful treatment requires a delicate approach to preserve natural facial expressions.
Typically, 3-5 injection points per eye are utilized, strategically placed to relax the orbicularis oculi without affecting eyelid function. Dosage usually ranges from 2-5 units per injection site, totaling 6-20 units per eye. Lower doses are often preferred initially, with potential for adjustments during follow-up appointments.
Careful consideration must be given to avoid diffusion to the upper eyelid, which can cause ptosis (drooping). Experienced injectors utilize shallow injection depths and precise targeting to minimize this risk. Patients should avoid rubbing the treated area for several hours post-procedure.
Lip Lines (Smoker’s Lines) ─ Precise Injection Techniques
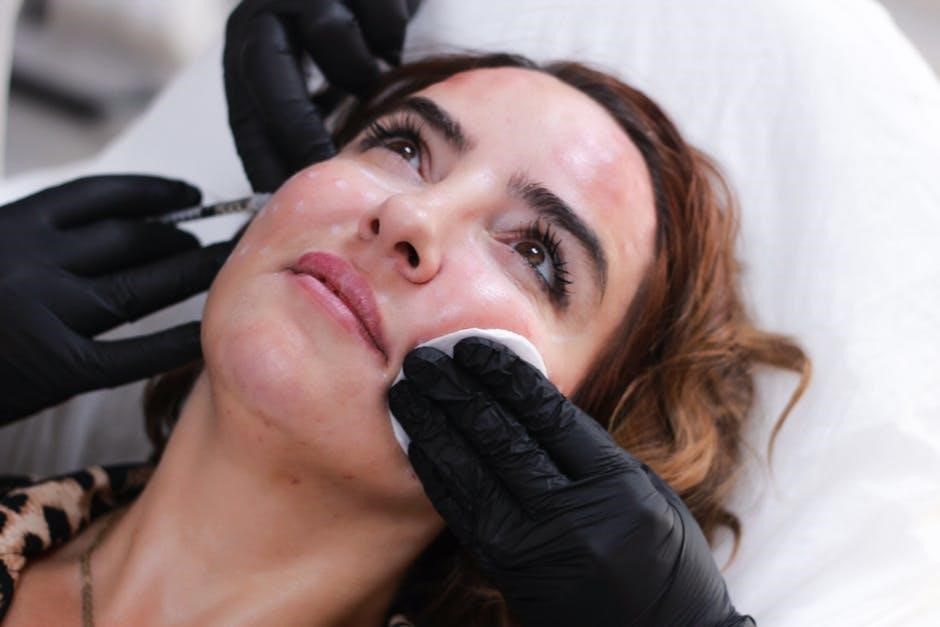
Addressing “smoker’s lines” – vertical lines around the mouth – with Botox requires meticulous technique. These lines are often a combination of dynamic wrinkles from muscle contraction (orbicularis oris) and static wrinkles due to collagen loss. Botox primarily targets the dynamic component, softening the appearance of lines during animation.
Injection points are carefully selected along the vermillion border (the edge of the lips) and into the orbicularis oris muscle. Dosage is typically low, ranging from 2-4 units per injection site, to avoid affecting lip movement or creating an unnatural appearance. A conservative approach is crucial.
Precise placement is paramount; injectors must avoid injecting directly into the lip tissue. Multiple small injections are preferred over a single larger dose to ensure even distribution and minimize the risk of asymmetry. Patient expectations should be managed, as Botox may not completely eliminate static lines.
Chin Dimpling (Mentalis Muscle) ─ Addressing Texture
Chin dimpling, caused by the mentalis muscle contracting, can be softened with strategic Botox injections. This treatment aims to relax the muscle fibers, reducing the appearance of the dimpled texture and creating a smoother chin profile. The mentalis muscle is located in the central chin area and is responsible for puckering the lips and creating the dimpling effect.
Injection points typically involve several small injections directly into the mentalis muscle. Dosage varies depending on the severity of the dimpling and individual muscle strength, generally ranging from 2-6 units per injection site. Careful assessment of the muscle’s activity during animation is essential for accurate placement.
The goal isn’t complete paralysis, but rather a subtle relaxation to minimize the dimpling without affecting natural facial expressions. Results typically last 3-6 months, requiring repeat treatments to maintain the desired effect.
Jawline Contouring (Masseter Muscle) ― Slimming Effect
Botox injections into the masseter muscle, located along the jawline, offer a non-surgical approach to jawline contouring and facial slimming. This technique reduces the muscle’s bulk, creating a softer, more defined jawline and a narrower facial appearance. The masseter muscle is primarily responsible for chewing.
Injection sites typically involve multiple points within the muscle, carefully avoiding nearby nerves. Dosage generally ranges from 20-30 units per side, adjusted based on muscle size and desired slimming effect. Precise placement is crucial to avoid affecting chewing function.
Over time, the muscle atrophies, resulting in a more sculpted jawline. Results typically last 4-6 months, with continued treatments potentially leading to longer-lasting muscle reduction. It’s important to note that this procedure can also alleviate symptoms of TMJ disorder.
Beyond Facial Aesthetics: Medical Applications of Botox
Beyond cosmetic uses, Botox effectively treats conditions like hyperhidrosis, migraines, bladder overactivity, strabismus, and cervical dystonia, showcasing its diverse therapeutic potential.
Hyperhidrosis (Excessive Sweating) ― Treatment Areas (Axillae, Palms, Soles)
Botox presents a highly effective solution for managing hyperhidrosis, characterized by abnormally excessive sweating. Treatment commonly targets the axillae (underarms), offering significant and lasting dryness. The procedure involves strategically injecting small doses of botulinum toxin into the affected area, temporarily blocking the nerve signals responsible for activating sweat glands.
Beyond the axillae, Botox is also utilized to treat palmar (palms) and plantar (soles) hyperhidrosis, though these applications often require a more meticulous injection technique and potentially higher dosages due to the greater muscle mass and nerve density. Successful treatment can dramatically improve quality of life, reducing discomfort and social anxiety associated with excessive sweating. Patients typically experience noticeable results within a few days, with effects lasting several months before repeat injections are needed. Careful assessment and precise injection placement are crucial for optimal outcomes and minimizing potential side effects.
Migraine Treatment ― Specific Injection Sites
Botox has emerged as a valuable therapeutic option for chronic migraine sufferers, receiving FDA approval for this purpose. The treatment protocol, known as the HEAD (Head and Neck Accupressure) protocol, involves a series of injections strategically administered to specific sites around the head and neck. These injection points target muscles frequently implicated in migraine pathogenesis, aiming to reduce muscle tension and nerve transmission involved in pain pathways.
Key injection sites include the temporalis muscles (temples), the occipitalis muscles (back of the head), the trapezius muscles (upper shoulders), and the cervical paraspinal muscles (neck). Precise placement, guided by anatomical knowledge, is essential for maximizing efficacy and minimizing discomfort. The treatment is typically repeated every three months to maintain consistent pain relief. While not a cure, Botox can significantly reduce the frequency and severity of migraine headaches, improving patients’ overall quality of life.

Bladder Overactivity (Neurogenic & Idiopathic) ─ Injection Protocol
Botox offers a compelling treatment avenue for both neurogenic and idiopathic overactive bladder (OAB), characterized by urgency, frequency, and involuntary urine leakage. The underlying principle involves relaxing the detrusor muscle – the bladder’s primary muscle responsible for contraction – thereby increasing bladder capacity and reducing uncontrolled spasms.
The injection protocol utilizes a cystoscopic approach, where Botox is directly injected into the detrusor muscle via a flexible cystoscope. Typically, around 20-30 units of Botox are distributed evenly throughout the bladder, avoiding the trigone area to preserve bladder emptying function. The procedure is generally performed under local anesthesia with or without sedation. Effects typically last for 6-9 months, requiring repeat injections to sustain symptom control. Careful patient selection and post-procedure monitoring are crucial for optimal outcomes and minimizing potential complications like urinary retention.
Strabismus (Crossed Eyes) ― Ocular Muscle Targeting
Botox presents a refined therapeutic option for strabismus, commonly known as crossed eyes, by selectively weakening overactive extraocular muscles. This approach aims to restore proper eye alignment and binocular vision. Precise injection targeting is paramount, guided by a thorough assessment of which muscle(s) contribute to the misalignment.
Typically, Botox is injected directly into the belly of the affected muscle – often the medial rectus for esotropia (inward turning) or the lateral rectus for exotropia (outward turning). Dosage varies based on muscle size and severity of the deviation, generally ranging from 1-5 units; The effect isn’t immediate, taking several days to weeks to manifest. Repeat injections are often necessary as the effect diminishes, typically lasting 3-6 months. Careful monitoring is vital to prevent overcorrection and ensure optimal visual outcomes.
Cervical Dystonia (Neck Spasms) ― Muscle Selection
Botox effectively manages cervical dystonia, characterized by involuntary neck muscle contractions, by selectively weakening the overactive muscles responsible for abnormal head postures. Precise muscle selection is crucial for optimal therapeutic benefit and minimizing functional impairment. Common target muscles include the sternocleidomastoid, trapezius, splenius capitis, and levator scapulae.
Injection sites are determined through careful palpation and observation of the patient’s head position during spasms. Dosage varies significantly, ranging from 50-500 units per treatment session, distributed among multiple muscles. Electromyography (EMG) guidance can enhance accuracy. Relief typically begins within a few days, lasting 3-4 months. Repeated injections are standard, with potential for developing antibodies reducing long-term efficacy. A comprehensive neurological evaluation is essential before initiating treatment.
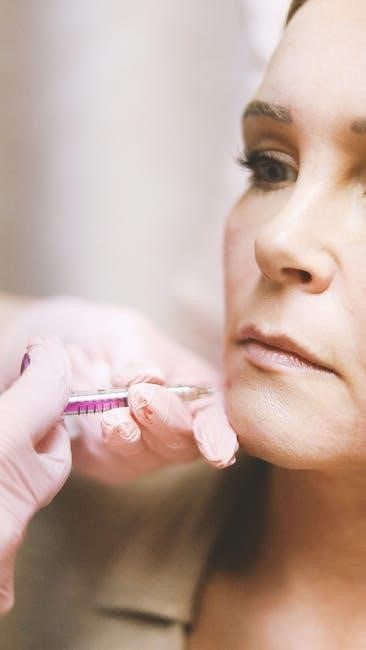
Technical Aspects of Botox Administration
Successful Botox injections demand meticulous technique, encompassing precise dosage calculations, appropriate dilution protocols, and careful consideration of injection depth and anatomical landmarks.
Botox Dosage & Dilution ― Standard Practices
Establishing standardized Botox dosage and dilution protocols is paramount for both efficacy and patient safety. While variations exist based on individual anatomy, treatment area, and product formulation, general guidelines prevail. Typically, Botox is reconstituted with sterile saline solution – often 0.9% sodium chloride – without preservatives.
The concentration for aesthetic applications generally ranges from 20 to 40 units per 0.1 mL, though this can be adjusted. For conditions like hyperhidrosis or bladder overactivity, lower concentrations might be employed. Accurate unit measurement is crucial, utilizing appropriately calibrated syringes. Dilution ensures even distribution and minimizes the risk of localized concentrations. Careful record-keeping of the dilution ratio and total units administered is essential for consistent results and potential adverse event tracking. Experienced practitioners tailor dosages based on muscle mass, desired effect, and prior treatment history.
Injection Depth & Angle ─ Anatomical Considerations
Precise injection depth and angle are fundamental to successful Botox administration, directly impacting both efficacy and minimizing off-target effects. Understanding underlying facial anatomy – muscle layers, nerve pathways, and vascular structures – is non-negotiable. Generally, injections target the neuromuscular junction, requiring a superficial intramuscular approach.
The ideal depth typically ranges from 2-4 mm, but varies depending on the muscle being treated. For example, glabellar lines necessitate a slightly deeper injection than periorbital wrinkles. Injection angles also differ; a more perpendicular approach is often used for superficial muscles, while oblique angles may be preferred for deeper targets. Avoiding intravascular injection is critical, necessitating slow injection rates and aspiration before injection. Thorough anatomical knowledge, coupled with careful technique, ensures accurate placement and optimal results.
Needle Gauge & Size ― Optimizing Comfort & Accuracy
Selecting the appropriate needle gauge and size is crucial for patient comfort and achieving precise Botox delivery. Finer gauges (30G-34G) are generally preferred, minimizing discomfort and reducing the risk of post-injection bruising. However, smaller gauges may require increased injection pressure, potentially leading to less accurate placement.
Needle length is determined by the injection depth required for the specific muscle target. Shorter needles (4mm-6mm) are suitable for superficial muscles like those around the eyes, while longer needles (8mm-13mm) may be necessary for deeper muscles like the masseter. Utilizing high-quality needles ensures smooth penetration and minimizes tissue trauma. Careful consideration of both gauge and length, tailored to the anatomical location and patient factors, optimizes both comfort and accuracy during Botox administration.
Post-Injection Care & Precautions
Following Botox treatment, patients should adhere to specific post-injection guidelines to maximize results and minimize potential complications. Avoid rubbing or massaging the treated areas for at least 24 hours to prevent toxin migration. Strenuous exercise should also be avoided for the same duration, as it can increase blood flow and potentially affect product distribution.
Patients are generally advised to remain upright for several hours post-injection to further minimize the risk of drooping. Over-the-counter pain relievers can manage any mild discomfort. It’s crucial to report any unusual symptoms, such as excessive swelling, bruising, or vision changes, to the administering physician immediately. Following these precautions ensures optimal treatment outcomes and patient safety.

Potential Risks & Side Effects of Botox
Common side effects include localized bruising, temporary swelling, and mild headaches; however, serious complications are rare, demanding immediate medical attention if they occur.
Common Side Effects (Bruising, Swelling, Headache)
Following Botox injections, experiencing mild and temporary side effects is quite common and generally resolves within a few days. Bruising at the injection site is perhaps the most frequently reported effect, stemming from minor blood vessel disruption during the procedure. Applying ice packs can help minimize bruising and swelling.
Localized swelling is also typical, particularly immediately after treatment, and usually subsides within 24-48 hours. Some individuals report experiencing a mild to moderate headache, often described as a tension-type headache, which typically responds well to over-the-counter pain relievers.
Redness and tenderness at the injection sites are also possible, but generally short-lived. These side effects are usually indicative of the body’s natural response to the injection and do not signify a serious complication. Patients should follow post-injection care instructions provided by their practitioner to optimize recovery and minimize discomfort.
Rare but Serious Complications ─ Addressing Concerns
While Botox is generally considered safe, rare but serious complications can occur, necessitating prompt medical attention. Ptosis, or eyelid drooping, can happen if the toxin diffuses into muscles controlling eyelid elevation, though this is usually temporary. Similarly, brow asymmetry can arise from uneven toxin distribution.
More concerning, though extremely rare, are allergic reactions manifesting as hives, difficulty breathing, or swelling. These require immediate emergency care. Additionally, distant spread of toxin effects, causing botulism-like symptoms such as muscle weakness, difficulty swallowing, or blurred vision, is a very rare but potentially life-threatening complication.
Proper practitioner training, accurate dosage calculation, and careful injection technique significantly minimize these risks. Patients should immediately report any unusual or worsening symptoms to their healthcare provider. Thorough pre-treatment evaluation to identify contraindications is also crucial for patient safety.
Contraindications for Botox Treatment
Certain conditions preclude Botox treatment to ensure patient safety. Active neuromuscular disorders like Myasthenia Gravis or Lambert-Eaton syndrome increase the risk of adverse effects due to enhanced sensitivity to the toxin. Existing infections at the injection site also represent a contraindication, as Botox could spread the infection.
Pregnancy and breastfeeding are absolute contraindications, as the effects of Botox on fetal development or infants are unknown. Patients with known hypersensitivity to botulinum toxin or any excipients in the formulation should avoid treatment.
The use of certain medications, such as aminoglycoside antibiotics, can also interfere with Botox’s action, increasing the risk of complications. A comprehensive medical history review is essential to identify these contraindications and ensure appropriate patient selection, minimizing potential risks and maximizing treatment outcomes.